Fall Prevention for Seniors: The Complete Home Safety Guide
Evidence-based fall prevention strategies for seniors covering home modifications, exercise, medication management, and environmental hazard reduction.


The Fall Prevention Crisis: Why This Matters Now
We have spent years analyzing home safety, and one fact stands out above the rest. The transition from independent living to assisted care is often triggered by a single, split-second event. Falls remain the leading cause of injury and injury-related death among adults 65 and older in the United States.
One in four seniors reports a fall every year. These incidents result in broken hips, traumatic brain injuries, and a sudden loss of confidence. A 2024 report from the CDC indicates that fall death rates are actually increasing, making this a critical issue for families to address immediately.
The financial impact is equally severe. Fall-related injuries now cost the U.S. healthcare system over $50 billion annually. For a typical family, a hip fracture can lead to medical costs ranging from $35,000 to $50,000, not including the long-term costs of rehabilitation or home care.
But we want to offer a different perspective on these statistics. Most falls are preventable with the right strategy.
Our experience confirms that a proactive approach can reduce fall risk by 30% to 50%. We have compiled this guide to cover the specific, evidence-based modifications and habits that actually work.
Understanding Why Seniors Fall
Falls are rarely caused by “clumsiness” or a simple accident. They are almost always the result of intrinsic (personal) and extrinsic (environmental) factors colliding at the wrong moment.
Intrinsic Risk Factors
We look at intrinsic factors as the internal changes that reduce a person’s margin for error.
| Factor | The Specific Risk | Prevalence |
|---|---|---|
| Muscle weakness | Sarcopenia (muscle loss) prevents correcting a stumble. | 40% of seniors |
| Balance disorders | Vestibular issues make “up” and “down” feel unreliable. | 35% of seniors |
| Vision problems | Cataracts and glaucoma hide tripping hazards. | 30% of seniors |
| Medication side effects | Blood pressure drops cause dizziness upon standing. | 25% take 4+ medications |
| Cognitive impairment | Slows the reaction time needed to grab a rail. | 15% of seniors |
| Chronic conditions | Neuropathy (foot numbness) hides uneven ground. | 80% have 1+ chronic condition |
| Fear of falling | Causes stiff movement, which ironically causes falls. | 30-50% of seniors |
Extrinsic Risk Factors
Extrinsic factors are the external hazards that we can physically remove or alter.
- Lighting Quality: Bulbs below 3000K (warm yellow) often hide edges; aging eyes need 5000K (daylight) for contrast.
- Throw Rugs: Unsecured mats are the number one tripping hazard in most homes.
- Bathroom Transfers: Stepping over high tub walls without grab bars.
- Stair Visibility: Wood steps that blend into wood floors without contrasting tape.
- Footwear: Walking in socks or loose slippers on hardwood.
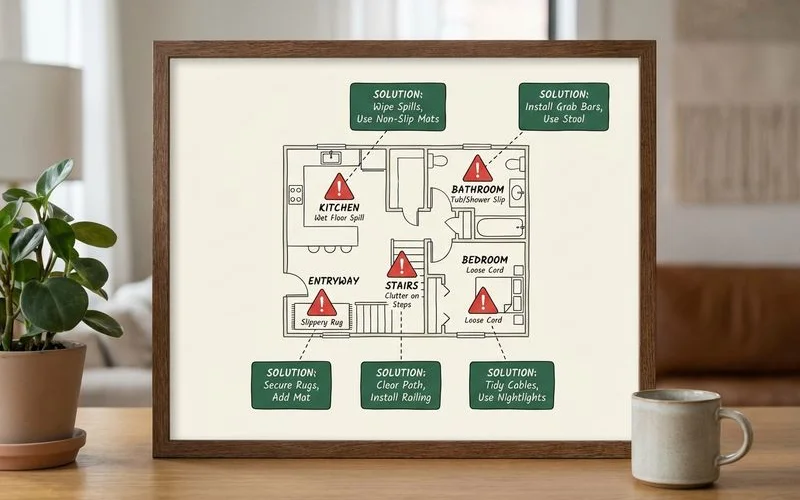 Most in-home falls occur in predictable locations that can be proactively addressed
Most in-home falls occur in predictable locations that can be proactively addressed
Strategy 1: Home Environment Modifications
Environmental modifications deliver the fastest return on investment for safety. You can eliminate roughly one-third of fall risks in a single weekend by addressing the “hot zones” in a house.
High-Priority Modifications
Bathroom (The Danger Zone): The combination of water, hard surfaces, and difficult transfers makes this the most dangerous room.
- Install professional grab bars: Do not rely on suction-cup handles, which can detach under weight. We recommend peened (textured) stainless steel bars screwed directly into studs.
- Upgrade lighting: Swap standard bulbs for high-lumen, cool-white LEDs to reduce shadows in the shower.
- Modify the toilet: Install a “comfort height” toilet (17-19 inches) or a riser. This reduces the leg strength needed to stand up.
- Shower safety: Use a transfer bench that allows the user to sit down outside the tub and slide in.
- Tub removal: If the budget allows, a walk-in tub or a zero-threshold shower eliminates the tripping hazard of the tub wall entirely.
Stairs and Hallways: Stairs are the location of the most severe injuries.
- Two-hand support: Install continuous handrails on both sides of the staircase.
- Grip size matters: Ensure rails are 1.25 to 1.5 inches in diameter so a senior’s hand can wrap fully around them.
- Visual cues: Apply high-contrast non-slip tape (like bright yellow or grey) to the edge of every step.
- Mechanical assistance: For multi-story homes, a stair lift is often safer and cheaper than moving to a new house.
Bedroom: Falls here often happen at night when seniors rush to use the restroom.
- Lighting paths: Install motion-sensing night lights along the baseboards from the bed to the toilet.
- Bed height: Adjust the bed so the mattress top is 20 to 23 inches from the floor. The user’s feet should be flat on the floor when sitting on the edge.
- Clear the path: Remove piles of laundry, cords, or furniture that encroach on the walking path.
Kitchen:
- Storage logic: Move heavy or daily-use items to waist-level shelves to prevent reaching or bending.
- Floor friction: Verify that kitchen mats have a high Coefficient of Friction (COF) rating or are taped down explicitly.
- Cabinet updates: Retrofit lower cabinets with pull-out drawers.
General:
- Rug removal: We strongly advise removing all throw rugs. If aesthetics are a priority, use double-sided carpet tape to secure them permanently.
- Floor transitions: Install beveled transition strips where carpet meets hardwood to smooth out the ridge.
We recommend using a structured checklist to catch every detail. You can use our DIY home safety assessment guide to perform a room-by-room audit.
Strategy 2: Exercise and Physical Activity
We often see families focus solely on the house, but the body needs reinforcement too. Research confirms that structured exercise programs reduce fall risk by 23% to 40%. The most effective protocols focus specifically on balance and leg strength.
Recommended Exercise Types
Balance Training: This is the specific skill of recovering when stability is lost. The CDC recommends the Otago Exercise Program, a series of strength and balance retraining exercises delivered by physical therapists. Tai Chi is another evidence-based practice that has been proven to reduce falls by improving body awareness.
Strength Training: Muscles deteriorate with age, a condition known as sarcopenia. Strengthening the quadriceps and glutes allows a senior to “catch” themselves during a stumble. Simple functional movements, like sit-to-stands from a sturdy chair, are incredibly effective.
Walking: Walking is excellent for heart health, but we must offer a caveat. Walking alone does not significantly reduce fall risk. It must be combined with balance training to be effective. Aim for 30 minutes of activity most days, but prioritize the balance component.
 Regular balance and strength exercises reduce fall risk by up to 40 percent
Regular balance and strength exercises reduce fall risk by up to 40 percent
Getting Started Safely
- Medical clearance: Always get a doctor’s approval before starting new physical exertions.
- Professional guidance: Ask a doctor about a referral for the “STEADI” initiative (Stopping Elderly Accidents, Deaths, and Injuries), which creates personalized plans.
- Start seated: Perform knee extensions and ankle pumps while sitting to build a baseline safely.
- Community resources: Local senior centers often host “SilverSneakers” classes designed specifically for stability.
Strategy 3: Medication Management
Medications are a silent contributor to instability. We find that seniors taking four or more prescriptions (polypharmacy) face a drastically higher risk of falling.
High-Risk Medication Categories
The American Geriatrics Society publishes the Beers Criteria, a list of medications that are potentially inappropriate for seniors. The following categories require extra vigilance.
| Category | Common Examples | The Fall Mechanism |
|---|---|---|
| Sedatives/Sleep Aids | Ambien (Zolpidem), Xanax | Causes “hangover” grogginess and slow reflexes. |
| Blood Pressure Meds | Lisinopril, Metoprolol | Causes Orthostatic Hypotension (dizziness upon standing). |
| Anticholinergics | Benadryl (Diphenhydramine) | Often causes confusion, blurred vision, and sedation. |
| Opioids | OxyContin, Vicodin | Significantly impairs balance and cognitive alertness. |
| Diabetes Meds | Insulin, Glipizide | Hypoglycemia (low blood sugar) leads to fainting. |
Action Steps
- The “Brown Bag” Review: Once a year, put all pill bottles in a bag and take them to a pharmacist. Ask specifically, “Do any of these interact to cause dizziness?”
- Deprescribing: Ask the doctor if any medications can be reduced or eliminated.
- Timing: Take sedating medications immediately before bed, not while still active in the evening.
- Transition protection: Fall risk is highest in the two weeks after a medication change. This is the ideal time to utilize a medical alert system for backup.
Strategy 4: Vision Care
Vision guides every step we take. Approximately one-third of all senior falls are linked to vision deficits. It isn’t just about blurriness; it is about contrast and depth perception.
Essential Vision Steps
- Bifocal Warning: Bifocals and progressive lenses can distort depth perception when looking down at feet. We recommend getting a dedicated pair of single-vision glasses specifically for walking outdoors or navigating stairs.
- Contrast Sensitivity: As eyes age, distinguishing between similar colors becomes difficult. Paint thresholds and door frames in contrasting colors to make them “pop.”
- Cataract Surgery: Do not delay this procedure. Studies show that cataract surgery can reduce the fall rate in seniors by over 30%.
- Manage Transitions: It takes aging eyes longer to adjust to light changes. Add extra lighting in entryways where a senior walks from bright sun into a dimmer hallway.
Strategy 5: Assistive Devices and Technology
We view assistive devices not as signs of weakness, but as tools of independence. The right gear keeps a senior mobile and safe.
Mobility Devices
- Canes: A standard cane helps with mild balance issues. For more stability, look for a “quad cane” with four feet.
- Rollators: Standard walkers require lifting, which can be tiring. A rollator (walker with wheels and brakes) provides smoother movement and includes a seat for resting.
- Proper Footwear: The ideal shoe has a low heel, a thin but firm midsole for ground feel, and a slip-resistant tread. Velcro closures are safer than laces that can untie.
Technology Solutions
- Wearable Detection: Modern devices like the Apple Watch and specific medical pendants now include accelerometers that detect hard falls and call 911 automatically.
- Smart Home Automation: Sensors can turn on lights automatically when a person puts their feet on the floor at night.
- Remote Monitoring: Systems can track daily activity patterns. If the bathroom door hasn’t opened by 9:00 AM, the system alerts a family member.
You can explore these options further in our detailed guide on smart home devices for aging in place.
The Fear of Falling Cycle: We often see seniors limit their movement because they are afraid of falling. This inactivity causes muscles to atrophy, which ironically increases the actual risk of a fall. Breaking this cycle requires building confidence through safety modifications and strength training.
Creating a Personalized Fall Prevention Plan
The most effective plan is one that is tailored to a specific home and health profile. We use this framework to help families get organized.
- Run the Audit: Use our DIY home safety assessment guide to identify the physical hazards in the home today.
- Consult the Pharmacist: Schedule a medication review specifically looking for the “Beers Criteria” risks.
- Check the Eyes: Ensure the prescription is current and ask about single-vision glasses for walking.
- Start the Movement: Enroll in a balance class or see a physical therapist for a custom home routine.
- Prioritize the Bathroom: Install grab bars and non-slip mats immediately; do not wait for a renovation.
- Review Regularly: Re-assess the home every six months or after any change in health status.
Fall prevention is an ongoing process, not a one-time fix. Our fall prevention and home modification services can help you implement these strategies with expert guidance. We know that taking these steps pays off in preserved independence and peace of mind for the entire family.
Ready to Take Action?
Learn more about our comprehensive fall prevention solutions and how they can help your family.
Explore Fall Prevention
About James Wilson
Home Safety Specialist & Accessibility Consultant
Certified home safety specialist with 10+ years designing accessible living spaces for seniors and individuals with mobility challenges.
Related Articles

DIY Home Safety Assessment: Room-by-Room Senior Guide
Learn to conduct your own home safety assessment with our detailed room-by-room guide. Identify fall hazards, accessibility issues, and safety improvements.

Where and How to Install Grab Bars: Location Guide With Diagrams
Expert guide to grab bar placement in bathrooms, hallways, and bedrooms. Includes installation heights, recommended products, and DIY vs. professional advice.
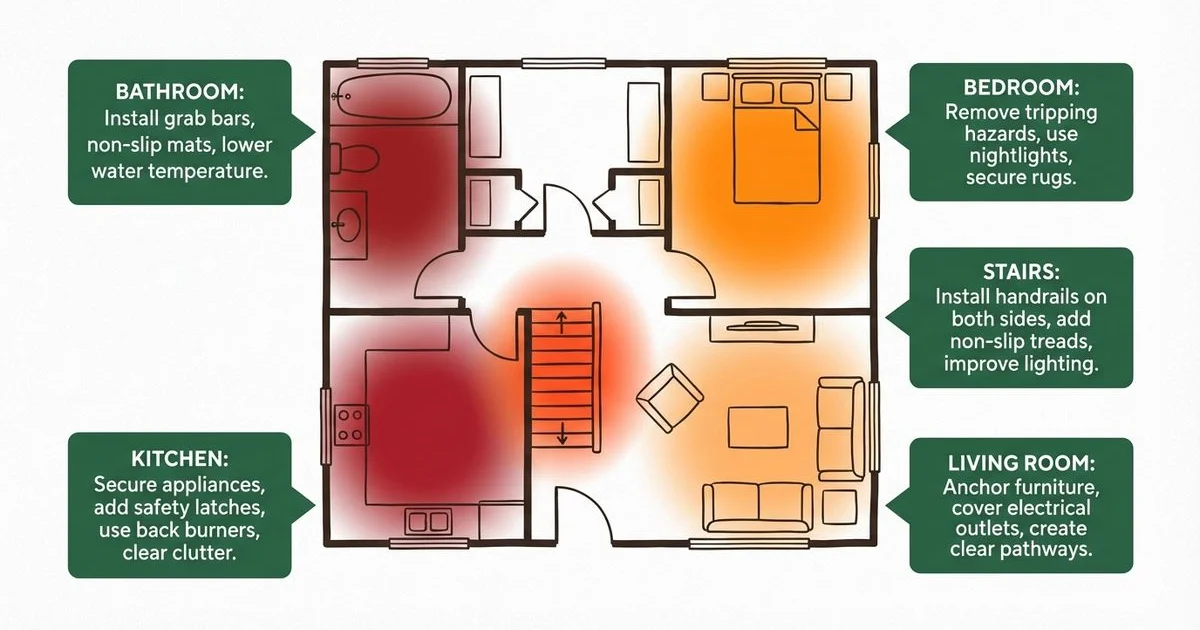
The 5 Most Dangerous Rooms in Your Home for Seniors (and How to Fix Them)
Discover which rooms pose the greatest fall and injury risks for seniors, with specific modifications to make each room safer.